A new study finds no evidence of benefit from a malaria drug widely promoted as a treatment for coronavirus infection.
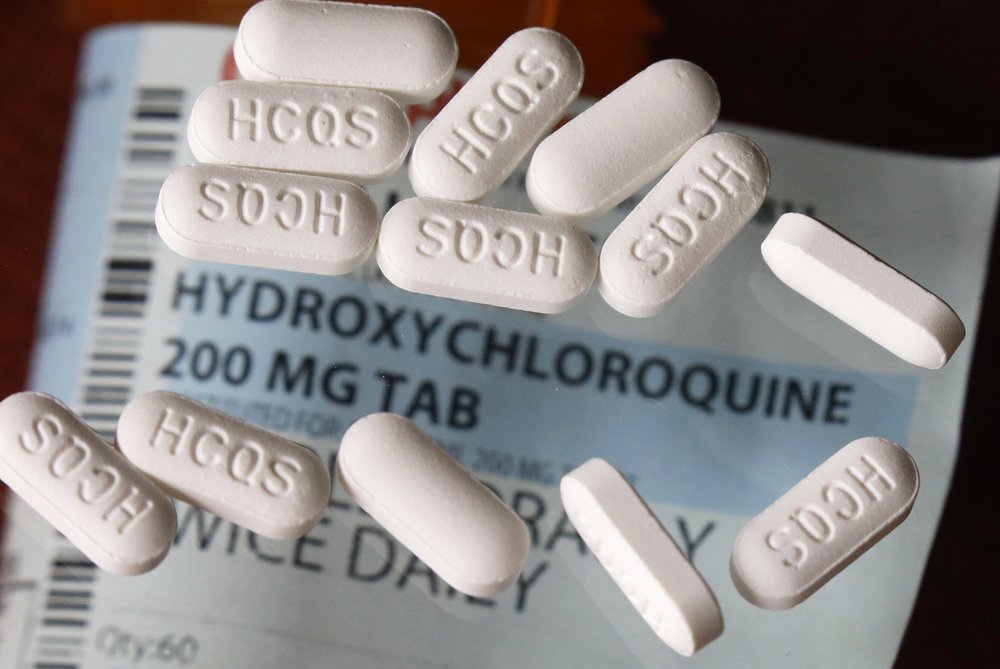
Hydroxychloroquine did not lower the risk of dying or needing a breathing tube in a comparison that involved nearly 1,400 patients treated at Columbia University in New York, researchers reported Thursday in the New England Journal of Medicine.
Although the study is observational rather than a rigorous experiment, it gives valuable information for a decision that hundreds of thousands of COVID-19 patients have already had to make without clear evidence about the drug’s risks and benefits, some journal editors and other doctors wrote in an editorial.
It is disappointing that several months into the pandemic, we do not yet have results” from any strict tests of the drug, they wrote. Still, the new study “suggests that this treatment is not a panacea.”
President Donald Trump repeatedly urged the use of hydroxychloroquine, which is used now for lupus and rheumatoid arthritis. It has potentially serious side effects, including altering the heartbeat in a way that could lead to sudden death.
The U.S. Food and Drug Administration has warned against its use for coronavirus infections except in formal studies.
Doctors at Columbia tracked how 565 patients who did not get the drug fared compared to 811 others who received hydroxychloroquine with or without the antibiotic azithromycin, a combo Trump also has touted.
In all, 180 patients required breathing tubes and 232 died, and the drug did not seem to affect the odds of either.
Patients given hydroxychloroquine were generally sicker than the others, but widely accepted methods were used to take that into account and still no benefit was seen for the drug.
Its use started within two days of admission for nearly all who received it. Some critics of earlier studies have said treatment may have started too late to do any good.
The study was funded by the National Institutes of Health, which has launched two of its own trials comparing hydroxychloroquine to placebo — the gold standard for establishing safety and effectiveness.
One study involves COVID-19 patients, and the other aims to see whether the drug can help prevent infections in health care workers exposed to the virus. Both got started in April.
